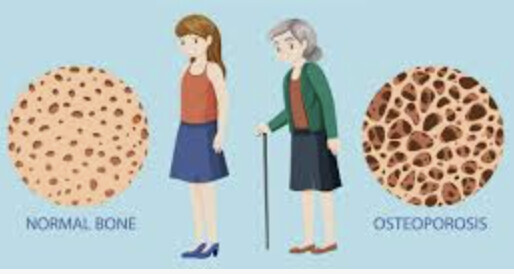
Osteoporosis is not something that happens suddenly. It is the slow, silent result of years of inadequate hormone support, and it begins far earlier than most women realize. By the time a fracture happens, significant bone loss has already occurred. The good news is that bioidentical hormone therapy is one of the most powerful tools we have for preserving skeletal integrity, and when started at the right time, it can stop bone loss in its tracks.
Why Estrogen Is Your Skeleton's Best Friend
Estrogen regulates the activity of osteoclasts, the cells responsible for breaking down old bone tissue, and supports the function of osteoblasts, the cells that build new bone. When estrogen levels are robust, bone remodeling stays in balance. When estrogen declines, osteoclast activity accelerates while osteoblast function slows down, creating a net loss of bone density year after year. In the first five to seven years following the final menstrual period, women can lose anywhere from ten to twenty percent of their bone mass. This is not a gradual, manageable decline. It is a significant structural change happening inside your body while you feel nothing at all. The vertebrae, hip, and wrist are particularly vulnerable because they are rich in the trabecular bone that responds most acutely to estrogen loss. Transdermal estradiol, particularly when delivered as BiEst combining estradiol and estriol, effectively maintains bone density in postmenopausal women. Research published in the New England Journal of Medicine and numerous subsequent trials has confirmed that women on estrogen therapy have significantly lower fracture rates than those not using hormones.
The Role of Progesterone in Building Bone
What is often overlooked in the osteoporosis conversation is progesterone. Natural progesterone, the bioidentical form, actually stimulates osteoblast activity. This means it does not merely slow bone loss the way estrogen does. It actively supports the formation of new bone. Research by Dr. Jerilynn Prior and others has documented progesterone's anabolic effect on bone tissue, which is one of the many reasons I include it as a foundational part of every hormone replenishment protocol. Synthetic progestins do not share this benefit. Medroxyprogesterone acetate, the progestin used in many conventional hormone regimens, does not have the same receptor affinity as natural progesterone and does not exert the same bone-building effects. This is one of many reasons why the distinction between bioidentical progesterone and synthetic progestins matters enormously.
Testosterone, DHEA, and Skeletal Strength
Testosterone is also critical for bone mineral density, in women as well as men. Androgen receptors are present throughout bone tissue, and testosterone supports cortical bone strength, which is the dense outer layer of bone. Women with low testosterone consistently show greater rates of bone loss and higher fracture risk. Restoring testosterone to an optimal physiological level is part of a comprehensive approach to skeletal protection. DHEA, which is produced in the adrenal glands and peaks in your mid-twenties before declining steadily with age, is a precursor to both estrogen and testosterone. Low DHEA is independently associated with reduced bone density and accelerated aging of the skeletal system. Including DHEA in a hormone replenishment protocol addresses the upstream hormonal environment that determines how well your bones can actually use the estrogen and testosterone you are providing.
What a DEXA Scan Tells You and What It Misses
A DEXA scan measures bone mineral density and compares it to the peak bone density of a young adult, expressed as a T-score. A T-score between zero and negative one is considered normal. Between negative one and negative 2.5 indicates osteopenia. Below negative 2.5 is osteoporosis. What a DEXA scan cannot tell you is the rate at which you are currently losing bone, which is why I also evaluate markers of bone turnover in lab work alongside a comprehensive hormone panel. Many of my patients come to me with borderline osteopenia and a doctor who told them to take calcium and come back in two years. Calcium supplementation without addressing the hormonal environment that governs bone remodeling is incomplete care. You cannot build a structurally sound house without the right foundation, and for your bones, that foundation is hormones.
When to Start and What to Expect
The earlier you begin hormone replenishment, the better the outcome for bone density. Starting in perimenopause, when the first drops in progesterone and then estrogen begin, allows you to preserve the bone mass you have before significant losses occur. Starting after menopause is still highly beneficial, particularly in the first decade, though it cannot fully reverse losses that have already happened. Women on a comprehensive bioidentical hormone protocol that includes estradiol, estriol, progesterone, testosterone, and DHEA typically show stable or improved bone density on follow-up DEXA scans. That is the standard of care I aim for with every patient. Fractures are not inevitable. They are largely preventable with the right hormonal foundation in place.
If you have been told to take calcium and come back in two years but nobody has looked at your hormones, that conversation is overdue. If you would like to discuss your hormones with someone who will take the full picture seriously, you are welcome to schedule a discovery call.
Dr. Anat Sapan, M.D. is a board-certified OB-GYN and menopause specialist practicing telemedicine in California, Florida, New York, and Illinois

Anat Sapan MD
Contact Me